As medical professionals, it is your responsibility to ensure that your patients get the best possible treatment. Additionally, you need to handle your money well if you want to run your operations and provide good service. One approach to fulfill this responsibility is to become an expert in Revenue Cycle Management (RCM). Revenue Cycle Management (RCM) is the lifeblood of healthcare companies’ financial well-being. In this article, we will go over what Revenue Cycle Management is, why it’s important, and the 13 stages to follow in order to adopt its successful methods.
Understanding Revenue Cycle Management
A healthcare organization’s performance hinges on its revenue cycle management. What follows is an explanation of revenue cycle management and how it works.
What is Revenue Cycle Management?
Revenue cycle management refers to the financial process that healthcare institutions use to monitor the income generated from patients during their whole experience, from their first appointment or consultation all the way to their final payment for the remaining amount. RCM integrates administrative data (such as a patient’s name, insurance provider, and other personal details) with clinical data (such as their treatment history and healthcare records) to bring the business and clinical aspects of healthcare together. Finding and fixing problems in the provider’s revenue cycle is what revenue cycle management is all about. Healthcare providers may earn more money from patient services and have more of their claims reimbursed with effective revenue cycle management.
Healthcare Revenue Cycle Management Process
A number of processes comprise RCM. These include reporting medical bills to insurance companies, coding procedures appropriately, translating medical services into billable costs, and collecting payments from patients for any unpaid amounts. The revenue cycle is essentially a multi-touchpoint commercial relationship with patients. The organization’s credibility might take a hit due to unnecessary rejections and bad debts, and patient and clinician satisfaction ratings can drop if these tasks are mismanaged.
Importance of Effective Revenue Cycle Management
An efficient RCM process in healthcare means that the whole patient engagement, from first inquiry to final payment, is well-managed. This ensures that the right data is gathered and recorded, that people are only charged for the services that were really rendered, that third-party payers are informed promptly, and that payments are collected.Improved patient satisfaction and financial gain may result from more efficient use of resources and fewer billing mistakes brought about by well-managed revenue cycles.
In addition to preventing them from having to make changes or resubmit the claim, this also helps providers understand why certain claims were refused and how to fix the problem. Furthermore, by automating tasks that were formerly performed by personnel, an RCM system may help healthcare businesses save time. Administrative responsibilities include communicating with patients about their scheduled appointments, keeping track of their current balances (both with payers and patients), and contacting insurers to inquire about particular issues related to rejected claims.
The 13 Steps of Revenue Cycle Management
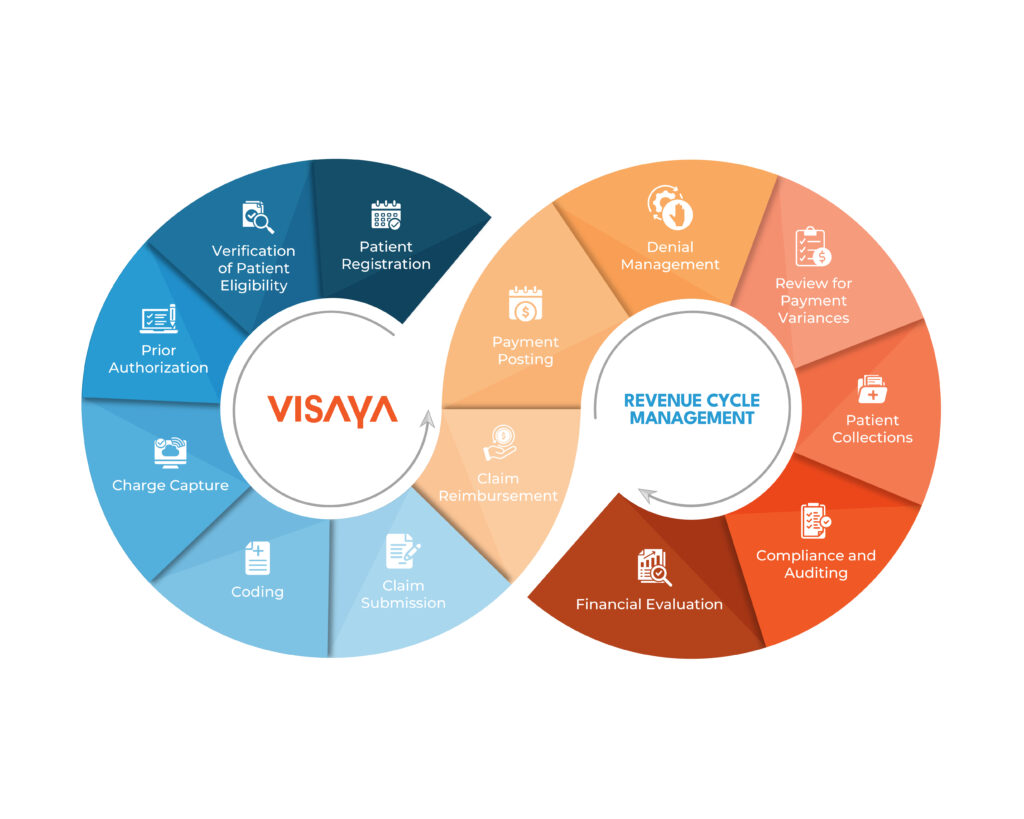
If healthcare providers want their payments on time, they need to follow the 13 phases of revenue cycle management. Here is a rundown of the 13 steps:
1. Patient Registration
Prior to a patient scheduling an appointment, the revenue cycle starts its initial stage. At the time of registration, the patient, their recommending doctor’s office, or a community organization supplies the necessary legal, financial, and insurance details. Punctual invoicing and trouble-free financial dealings are guaranteed by this. Incorporating automated technologies may help ensure accurate data, minimize mistakes, and streamline the process. Staff should also undergo regular training to ensure they are up-to-date on the newest data gathering procedures.
2. Verification of Patient Eligibility
Before you can find out the treatments a patient’s insurance will pay for, you must check the account’s insurance data. You should contact the patient in advance to keep the connection open and honest in the event that there is a problem in the verification procedure. Claims denials and payment delays are less likely to occur when patients’ eligibility is confirmed. It safeguards the healthcare professional and patient from unforeseen expenses by verifying that the patient’s insurance will pay the services rendered.
3. Prior Authorization
Authorization for procedures may be required once patients provide the required documentation to back up their claim. Just make sure you have enough documentation to back up your claim of medical need for these operations before you ask for prior authorization. Your patients will appreciate how easy it is to have prior authorizations automated, and they will likely continue to use your services as a result.
4. Charge Capture
During the charge entry process of medical billing, doctors and hospitals document the many services they provided to patients and submit the associated costs to their patients’ insurance companies. From the perspective of revenue cycle management, this metric is critical for ensuring that hospitals get their full reimbursement from insurance companies.
5. Coding
Accurate and up-to-date medical coding that accurately reflects the procedures the patient has had is crucial for proper reimbursement of your services. In order to stay accurate when coding standards change, it is recommended to undergo frequent audits and participate in continuous training. Also, look at how coding teams might benefit from AI tools that can boost efficiency.
6. Claim Submission
Submit the claim form to the insurance company after you have ensured that all the codes are correctly entered. Because claim denials and payment delays might result from mistakes or omissions, accuracy is paramount throughout this procedure. Achieving successful claim submission requires precise coding, comprehensive documentation, and strict adherence to criteria set by each payer. If you want to keep your healthcare finances stable and get paid on schedule, you need to streamline this phase.
7. Claim Reimbursement
After getting the claim, the insurance company will verify it in their system to determine the right compensation based on the patient’s coverage and their own discretion. In order to streamline the claim filing process in your RCM, you may take use of the explanations provided by most insurance carriers on the reimbursement amount.
8. Payment Posting
A crucial aspect of the process is posting payments, which involves recording and applying funds from patients, insurance companies, and third-party payers to their records. Claims reimbursements and payments must be promptly sent to the appropriate patient accounts as soon as they reach the office. Investigate any inconsistencies or underpayments and make sure your practice is submitting payments correctly and effectively.
9. Denial Management
If not handled quickly and efficiently, denied claims might result in a substantial loss of revenue. In this step, you should look into the rejections, fix the mistakes, and resubmit the claims to get your money back. If you want to know how to appeal a refusal, you need to know what causes them. Be careful to cover all bases, as this may involve anything from checking medical need to analyzing coding methods.
10. Review for Payment Variances
Several factors, including an absence of medical necessity or inaccurate classification of major/minor procedures, can cause the amount you get from your claim to differ from what you originally requested. After you receive the refund, check the amounts and submit an appeal to your insurance carrier with the required paperwork.
11. Patient Collections
One of the most important parts of any system for medical billing is this.It involves informing patients of their financial obligations, providing them with payment choices that are both flexible and efficient, and ultimately obtaining payments. Being patient and diligent is essential when following up with overdue payments. Have a conversation with them about payment plans or reductions that are available for timely payments if they are having trouble making payments for whatever reason.
12. Compliance and Auditing
Following that, you must carefully examine all thirteen stages of revenue cycle management to spot patterns and find ways to enhance them. Verifying and evaluating conformity with rules and regulations is what compliance and auditing are all about. In order to pinpoint exactly where improvement is needed, it is a good idea to monitor key performance metrics such as A/R days or denial rates.
13. Financial Evaluation
If healthcare revenue cycle management is to undergo continual development, it is essential to regularly report and analyze financial data to get insights into revenue trends. The purpose of financial reporting and analysis is to help in strategic decision-making by examining and interpreting financial data. If you want to get the most out of automating your revenue management system, make sure the RCM model you use generates analytical data.
Turn to VISAYA KPO for Your RCM Needs
If healthcare companies want to keep their finances in order, they need to master the 13 phases of revenue cycle management. In the dynamic field of medical billing and service supply, this all-encompassing strategy aims to maximize revenue flow, decrease inefficiencies, and enhance operational excellence.
Get in touch with VISAYA KPO if you want an assurance of the finest RCM model. You can rely on the team of specialists here to help you achieve your income goals. When you work with our team, we can tailor solutions to meet your specific needs. Contact us today if you’re interested in learning more about how we can help you improve your revenue cycle management.

